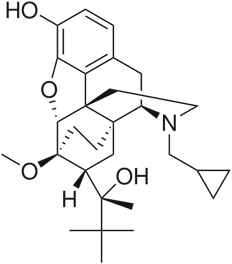
Buprenorphine
Buprenorphine is a semi-synthetic opioid analgesic used to treat opioid addiction as well as moderate acute and chronic pain. Although buprenorphine has been available since the 1980s, it was only in 2002 that it was approved by the FDA for use as an opioid-replacement therapy for individuals addicted to opioids.
When used by someone who is dependent on another opioid and not already in withdrawal, buprenorphine may trigger an extremely intense form of opioid withdrawal called "precipitated withdrawal." This is because buprenorphine binds more strongly to receptors in the brain than other opioids do, and when given in sufficient quantities, can block and reverse the effects of other opioids already present. This effect is very similar to the opioid antagonist drug naloxone, which is commonly used to counter the effects of an opioid overdose. Naloxone is also present in small quantities in Suboxone, a popular sublingual buprenorphine preparation used to treat opioid dependance.
Due to the chance of precipitated withdrawal, when buprenorphine is being used to treat addiction to other opioids, it is suggested that a person should wait until basic withdrawal symptoms appear before taking their first dose of buprenorphine.
Buprenorphine is also used recreationally, most commonly by insufflation (snorting) or injection. In addition to the euphoria and other effects common to most opioids, some recreational users report feeling a slight "upper"-like effect. Patients taking buprenorphine for addiction therapy have reported that obtaining euphoria is virtually impossible after the first few doses. Many users addicted to other opioid drugs will use buprenorphine to prevent withdrawal when they are unable to use their opioid of choice.
Brand Names
Suboxone, Subutex, Temgesic, Buprenex, Norspan, Butrans
Street Names
subs, bupe, stops, stop signs
Formulations
- Suboxone - sublingual film, buprenorphine/naloxone: 2 mg/0.5 mg, 8 mg/2 mg
- Temgesic - sublingual tablet, buprenorphine hydrochloride (HCl): 200 mcg
- Buprenex - injection solution, buprenorphine HCl: 300 mcg/mL
Medical Uses
- treatment of opioid dependance/addiction
- relief of acute and chronic moderate pain
Route of Administration
sublingual, intramuscular (IM), intravenous (IV), transdermal, insufflation (snorting), rectal
Half-life
20-70 h
Medical Dosage
- moderate pain: ~200 mcg injected (IV, IM) for acute, 20 to 70 mcg/h transdermal patch for chronic
- narcotic addiction maintenance: 4 to 24 mg sublingually per day. Patients are started at 2 to 8 mg per day and increased 2 to 4 mg per day until a stable dose is reached.
Legality
- Buprenorphine is a Schedule III drug in the United States. Buprenorphine was rescheduled in 2002 by the DEA from Schedule V to Schedule III.
- Buprenorphine is a Schedule I drug in the Canada.
Images
References
- About Buprenorphine Therapy. The Substance Abuse and Mental Health Services Administration (SAMHSA). buprenorphine.samhsa.gov, 2013.
- Schumacher MA, Basbaum AI, Way WL, Opioid Analgesics & Antagonists (Chapter 31) in: Basic and Clinical Pharmacology. 12e. Katzung BG, Masters SB, Trevor AJ (Editors). McGraw-Hill / Lange, 2012.
- Rosado J, Walsh SL, Bigelow GE, Strain EC. Sublingual buprenorphine/naloxone precipitated withdrawal in subjects maintained on 100mg of daily methadone. Drug and Alcohol Dependence Oct 2007; 90(2-3):261-9. [PubMed] [PDF]
- Johanson CE, Arfken CL, di Menza S, Schuster CR. Diversion and abuse of buprenorphine: findings from national surveys of treatment patients and physicians. Drug and Alcohol Dependence Jan 2012; 120(1-3):190-5. [PubMed]
- Diversion and Abuse of Buprenorphine: A Brief Assessment of Emerging Indicators, Final Report. Substance Abuse and Mental Health Services Administration (SAMHSA) / Center for Substance Abuse Treatment (CSAT), 2006. [PDF]
- Clinical Practice Guideline for Management of Opioid Therapy for Chronic Pain. United States Department of Veterans Affairs / Department of Defense, May 2010. [PDF]
- Controlled Substances - Alphabetical Order. DEA Office of Diversion Control, May 2013. [PDF]
- Controlled Drugs and Substances Act. Minister of Justice, Canada, Nov 2012. [PDF]
Related Pages
-
Buprenorphine Medication Identification
A list of imprints on buprenorphine medicines with images and details including dosages, manufacturer, shape, and color. -
Buprenorphine Treatment
What is buprenorphine (Suboxone, Subutex)? How does buprenorphine treat opioid addiction? Why is buprenorphine combined with naloxone? Learn about buprenorphine treatment, a relatively new method of medication-assisted treatment. -
Methadone
Methadone is a synthetic opioid that is most commonly used as a maintenance treatment for opioid addiction. Methadone is also used in managing severe chronic pain, due to its long duration of action, high potency, and very low cost. -
Methadone Maintenance
Methadone Maintenance Treatment (MMT) has been proven to be a safe and effective treatment for opioid dependence and addiction. Read about the history of methadone and how a methadone treatment program works.